Medical Library
Loading...Please Wait
Achilles Tendonitis and Rupture
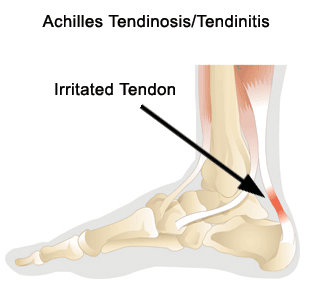
The Achilles tendon attaches the calf muscle (called the gastrocnemius and soleus muscles) to the heel. Excessive stress or a tight or fatigued calf muscle can result in microtrauma, degeneration, and even inflammation of the tendon- a condition called Achilles Tendonitis/Tendinosis. Prolonged walking, overtraining (excessive running or jumping, or walking hills can cause this condition.
Recent research suggests that a gradual onset of pain and prolonged recovery might be due to a similar condition called Achilles tendinosis. Tendinosis is chronic degenerative condition and it differs from tendonitis in that there is no inflammation present. It is probably more common than tendinitis because often times tendon pain is not accompanied by the classic inflammatory signs of swelling, redness, and warmth.
Treatment usually consists of rest, non-steroidal anti-inflammatory drugs (NSAIDs), ice, stretching, strengthening and progressive return to function or sport.
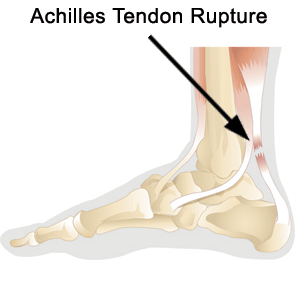
Forceful contraction of the calf muscle may rupture (completely tear) the Achilles tendon. It occurs during jumping, running, and cutting and is often seen in basketball and baseball players. The patient often reports the sensation of having been hit or violently kicked in the lower calf. There is pain and a “divot” in the tendon above the heel.
Treatment- non-surgical rehabilitation and surgical repair are viable treatment options. Active people may experience more benefit from surgical repair. Rehabilitation may require six to twelve months of progressive care.
Possible Treatments
- Ankle Active Range of Motion

- Ankle Joint Mobilization

- Ankle Joint Passive Range of Motion

- Ankle Progressive Resistive Range of Motion

- Aerobic/Endurance Exercise

- Cryotherapy or Cold Therapy

- Electrotherapeutic Modalities
- Gait or Walking Training

- Heat Pack

- Isometric Exercise

- Plyometrics

- Proprioception Exercises

- Physical Agents
- Soft Tissue Mobilization

- Stretching/Flexibility Exercise

Possible Treatment Goals
- Improve Balance
- Improve ability to bear weight/stand on the leg(s)
- Decrease Risk of Reoccurrence
- Improve Fitness
- Improve Function
- Improve Muscle Strength and Power
- Increase Oxygen to Tissues
- Improve Proprioception
- Decrease Postoperative Complications
- Improve Range of Motion
- Self-care of Symptoms
- Improve Wound Healing
Additional Resources
Disclaimer
The information in this medical library is intended for informational and educational purposes only and in no way should be taken to be the provision or practice of occupational therapy, medical, or professional healthcare advice or services. The information should not be considered complete or exhaustive and should not be used for diagnostic or treatment purposes without first consulting with your physical therapist, occupational therapist, physician or other healthcare provider. The owners of this website accept no responsibility for the misuse of information contained within this website.