Medical Library
Loading...Please Wait
Shoulder Instability
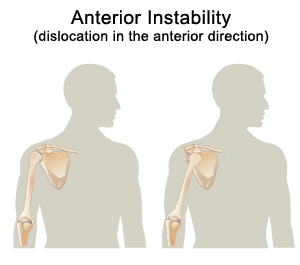
Shoulder instability occurs when the shoulder moves completely out of its socket (dislocation) and requires a medical professional to “relocate it”, or to a lesser degree, when it slips out of joint but spontaneously move back in place (subluxation). Usually, the shoulder dislocates or subluxes forward (this is called an anterior dislocation). Much less often, it dislocates backward (posterior dislocation), and sometimes, it can slip out forward, backward, or downward (this is called multidirectional instability). Remember, you may have an “unstable” shoulder that has not completely dislocated.
The shoulder is most at risk for anterior dislocation when the arm is placed in an abducted and external rotated position (such as a fall on the outstretched hand or tackling a player).
An anterior dislocation is obvious because it is immediately noticed by the person right after the trauma. However, minor instability may result in a sensation that the shoulder is slipping out of place with or without pain. One might also experience pain or a sense of “apprehension” when the arm is abducted and externally rotated (ask your physical therapist about this).
A sudden dislocation is an emergency. The patient should be taken to the emergency room immediately to make sure there is no damage to the blood vessels or nerve that go to the shoulder, arm, and hand. Usually, the emergency room physician can move the arm in such a way that the dislocated shoulder reduces back into its proper place. Rarely is surgery indicated. Pain and muscle relaxant medication is often prescribed. Ice can also help reduce the pain. Physical therapy is usually started 2-3 weeks after a dislocation to strengthen the muscles that support the shoulder joint.
Possible Treatments
- Active Assistive Range of Motion

- Aerobic/Endurance Exercise

- Core Strengthening

- Cryotherapy or Cold Therapy

- Electrotherapeutic Modalities
- Isometric Exercise

- Proprioceptive Neuromuscular Facilitation (PNF)

- Posture Training

- Proprioception Exercises

- Physical Agents
- Shoulder Active Range of Motion

- Shoulder Joint Mobilization

- Shoulder Passive Range of Motion

- Shoulder Resistive Range of Motion

- Soft Tissue Mobilization

Possible Treatment Goals
- Decrease Risk of Reoccurrence
- Improve Fitness
- Improve Function
- Optimize Joint Alignment
- Improve Muscle Strength and Power
- Increase Oxygen to Tissues
- Improve Proprioception
- Decrease Postoperative Complications
- Improve Relaxation
- Self-care of Symptoms
- Improve Safety
- Improve Tolerance for Prolonged Activities
Additional Resources
Disclaimer
The information in this medical library is intended for informational and educational purposes only and in no way should be taken to be the provision or practice of occupational therapy, medical, or professional healthcare advice or services. The information should not be considered complete or exhaustive and should not be used for diagnostic or treatment purposes without first consulting with your physical therapist, occupational therapist, physician or other healthcare provider. The owners of this website accept no responsibility for the misuse of information contained within this website.